Synergistic Effect
- An enhanced bone graft substitute composed of 45S5 bioactive glass, carbonate apatite anorganic bone mineral, and Type I collagen
- A combination that drives a synergistic effect to induce osteoblasts proliferation, matrix maturation, and extracellular matrix mineralization 1
Bioactive Glass
- 30% bioactive glass
- Promotes cell proliferation & differentiation 2
- 100-300pm particle Size 3,4,5
Carbonate Apatite
- Optimal resorption & remodeling-similar to human bone 6,7
- Pores provide pathways for cell migration and attachment to lay down new bone
- Higher osteoclastic & osteoblastic activity than BTCP & HA 8
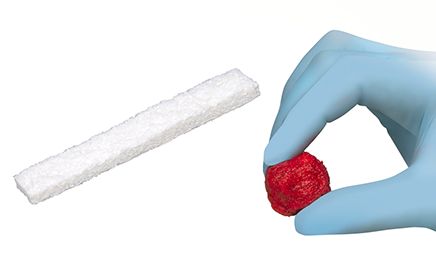
Type 1 Collagen
- Highly absorbent, moldable, flexible, and resists migration upon irrigation
- Binds proteins and cells and retains biological factors 9
- 100% resorbable through normal metabolic pathways 10
- Intrinsic hemostatic properties control minor bleeding 10,11
1. Ferreira, S.A., Young, G., Jones, J.R., Rankin, S. 2021. Bioglass/ Carbonate Apatite/ Collagen Composite Scaffold Dissolution Products Promote Human Osteoblast Differentiation. Materials Science & Engineering C, 118
2. Xynos, I.D., Hukkanen, M.V., Batten, J.J., Buttery, L.D.K. Hench, LL, Polak, J.M. (2000). Bioglass 4555 stimulates osteoblast turnover and enhances bone formation in vitro: Implications and applications for bone tissue engineering. Calcif Tissue Int. 67(4), 321-9.
3. Oonishi, H., Kushitani, S., Yasukawa, E., Iwaki, H., Hench, LL, Wilson, J., Tsuji, E., Sugihara, T. (1997). Particulate Bioglass Compared with Hydroxyapatite as a Bone Graft Substitute. Clinical Orthopaedics and Related Research, 334, 316-325, Lippincott-Raven Publishers, Philadelphia, PA
4. Schepers, E.J.G., Ducheyne, P. (1997). Bioactive glass particles of narrow size range for the treatment of oral bone defects: a 1-24 month experiment.
5. Lindfors, N. C., Koski, I., Heikkila, J., Mattila, K. and Aho, A J. (2010). A prospective randomized 14-year follow-up study of bioactive glass and autogenous bone as bone graft substitutes in benign bone tumors. J. Biomed. Mater. Res., 94B, 157-164. doi:10.1002/jbm.b.31636
6. Matsuura, A., Kubo, T. Doi K., Hayashi, K., Morita, K., Yokota, R., Hayashi, H., Hirata, 1. Okazaki, M., Akagawa, Y. (2009). Bone formation ability of carbonate.
7. Ellies, LG., Carter, J.M., Natiella, J.R., Featherstone, J.D.B., Nelson, D.G.A. (1988). Quantitative analysis of early in vivo tissue response to synthetic apatite implants. J. of Biomed. Mater. Res. 22. 137-148.
8. Kanayama, K., Sriar), W., Shimokawa, H., Ohya, K., Doi, Y., Shibutani, T. 2011. Osteoclast and Osteblast Activities on Carbonate Apatite Plates in Cell Cultures. J. Biomaterials, 26, 435-436.
9. Geiger, M., LI, R.H., Friess, W. (2003). Collagen sponges for bone regeneration with rhBMP-2. Science Direct/ Elsevier, 55, 1613-1629. http://doi.org/10.1016/j.addr.2003.08.010
10. LI, S.T. (2000). Biomedical Engineering Handbook, In JD Bronzino (Eds.), Biologic Biomaterials: Tissue Derived Biomaterials (Collagen) (1st ed.) 2, 42, 1-23, CRC Press, Boca Raton, FL
11. Jaffe, R., Deykin, D. (1974). Evidence for a Structural Requirement for the Aggregation of Platelets by Collagen. The Journal of Clinical Investigation, 53, 875-883.